Clinical Programming
The Global TB Program has focused on the seamless integration of TB and HIV care and treatment across our network of African partner sites and expanded efforts to support the eight clinical centers of excellence located in seven countries (BIPAI). The TB Program has also conducted trainings, improved standardization, and enhanced the existing Electronic Medical Records (EMR) system to effectively capture outcome data regarding TB and other common HIV-comorbidities.
Policy
In collaboration with colleagues from IUATLD, McGill University, and the Cochrane Collaboration, the Global TB Program partners to conduct systematic reviews and meta-analyze data to generate evidence informing international and WHO policy regarding the care and treatment of children battling TB. Examples of this work include the following publications:
Mandalakas A, Detjen A, Hesseling A, Benedetti A, Menzies D. Interferon-Gamma Release Assays for the detection of Mycobacterium tuberculosis infection in children: a systematic review and meta-analysis. International Journal of Tuberculosis and Lung Disease. 2011 Aug; 15(8):1018-32.
Detjen AK, DiNardo AR, Leyden J, Steingart KR, Menzies D, Schiller I, Dendukuri N, Mandalakas AM. Xpert MTB/RIF assay for the diagnosis of pulmonary tuberculosis in children: a systematic review and meta-analysis. The Lancet Respiratory Medicine. 2015 Mar 23. PubMed PMID: 25812968
DiNardo AR, Detjen A, Ustero P, Ngo K, Bacha J, Mandalakas AM. Culture is an imperfect and heterogeneous reference standard in pediatric tuberculosis. Tuberculosis. 2016 Sep 28. PMID: 27727131
Research
Partnering with institutions to provide linkage of new and established researchers, the Global TB Program has successfully attracted a new cadre of investigators to collaborate in TB-related research and expand capacity at our existing and newly established research centers. Learn more about the Global TB Program’s research.
Global TB Publications
View a listing of global tuberculosis related research articles in PubMed.
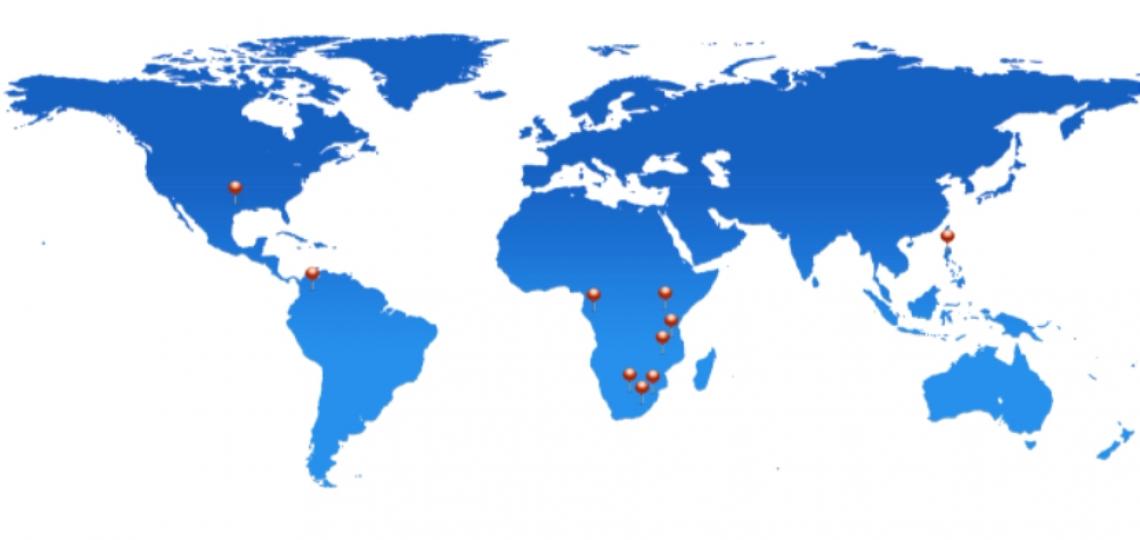
Where We Work

The Global TB Program’s focus in Botswana is to improve clinical conditions and knowledge about treating Pediatric TB. Our focus is on diagnostics, prevention and treatment, and infection control.
To improve diagnostics, we have collaborated with the University of Pennsylvania and District TB coordinators in institute contract tracing, developed a comprehensive Pediatric TB curriculum, trained HCWs on Pediatric TB and on proper sputum collection and sample handling, issued a nationwide roll-out of sputum induction and Gastric Aspiration, and engaged and lobbied CMS to ensure timely ordering of supplies. To improve the prevention and treatment of Pediatric TB, we have educated HCWs on the importance of Isoniazid Preventive Therapy (IPT) and IPT guidelines, trained HCWs on Pediatric TB diagnosis and treatment, implemented DOTS, and have an ongoing adherence counseling.
To improve the prevention and treatment of Pediatric TB, we have educated HCWs on the importance of IPT and IPT guidelines, trained HCWs on Pediatric TB diagnosis and treatment, implemented DOTS, and have an ongoing adherence counseling. To improve infection control, we have educated HCWs and the community on TB infection control and have conducted a health facility risk assessment.
To improve infection control, we have educated HCWs and the community on TB infection control and have conducted a health facility risk assessment.

The Global TB Program has been involved in increasing awareness for Pediatric TB in Colombia. Program staff participated in a workshop in Bogota, Colombia providing lectures on lessons learned from the successful Stop TB Partnership funded TB REACH project in eSwatini, the cost-effectiveness of IPT, TB in maternal and child health, and practical approaches for developing a TB Center of Excellence (COE). The workshop took place March 1-3, 2017. This workshop served to update/educate issues surrounding TB in the country and included clinicians, representatives from civil society, and National TB Program (MTP) managers from across the country. This was a joint effort organized with Baylor-Colombia and the International Organization on Migration (IOM) – Colombia that was hosted at the Ministry of Health Facility. Speakers included local and international experts from academia, WHO, and PAHO.

Houston
The Children’s TB Clinic at Texas Children’s Hospital cares for children in Houston, Texas. Services are provided for children with TB exposure, infection, and disease is cared for at this clinic.

The Global TB Program collaborated with the Translational research department and Baylor College of Medicine faculty members, Drs. Edith Mohapi and Jill Sanders, on a TB REACH project, Fumana TB Baneng, in Lesotho. Funded by the WHO, the project aimed to improve diagnosis and treatment of TB by increasing educational efforts among health care workers and improving sputum collection efforts.

The Global TB Program’s focus in Malawi is to improve clinical conditions and knowledge about treating Pediatric TB. The program's focus is on diagnostics, prevention and treatment, and infection control.
To improve diagnostics, they have increased sputum collection, developed a sputum collection SOP, visited CHSU and learned how to submit cultures, established a plan for Gene Xpert access, shared our chest x-ray training lecture with our staff, made use of radiology consultants, implemented monthly rounds of chest x-rays, implemented TB training at COE, incorporated curriculum into current attachment programs, provided HCW training, and created SOP for contact tracing.
To improve the prevention and treatment of Pediatric TB, they have convened a clinical discussion to determine the duration of IPT in pre-ART patients and have addressed reporting and drug forecasting with NTP in TWG setting.
To improve infection control, they have implemented screening questions in triage, created SOP for infection control, set aside a TB clinic day, set aside specific rooms to screen positive TB patients, and implemented cough screens and rooms.

The Global TB program worked under the 2014 expansion of Baylor College of Medicine and Texas Children’s Hospital in Papua New Guinea. The Global TB Program collaborated with Dr. Henry Welch and other faculty from the Papua New Guinea School of Medicine to improve care and treatment of families affected by TB.
One of these areas includes the development of postdoctoral projects in TB research. These projects focused on the areas of improving the diagnosis of TB in children, evaluating the utility of GeneXpert on gastric and fine needle aspirate samples in PNG children. Two paediatric trainees have been published, and one of them has presented at the International Union Against TB and Lung Disease
Over the last 4 years, the Global TB program has been working with the PNG Paediatric Society to introduce a new child-friendly TB medication. In December, 2015 a new child-friendly TB medication became available worldwide. In anticipation of this, the Global TB Program helped coordinate with local partners including the World Health Organization (WHO) the first ever national workshop in child TB. The workshop took place Nov. 2016 and served to update/educate issues surrounding pediatric TB and included clinicians from all 22 provinces in the country. Approximately 80 participants were in attendance including stakeholders from the Burnett Institute, World Vision, UNICEF, TB Alliance, MST, and Australian DFAT. In addition to the introduction of the new FDC, Dr. Anna Mandalakas lectured and met with local partners on the cost-effectiveness of isoniazid preventive therapy (IPT).
Working with the PNG Paediatric Society, PNG became the 1st country in the Western-Pacific Region, and the 4th country worldwide to introduce this medication under a locally owned and directed initiative known as the Child TB Project. This project is ongoing and is works toward improving diagnosis, care, treatment, and prevention for families with TB. Since its inception, the project has secured funding into its’ 4th year from the Australian DFAT and the Baylor International Pediatric Aids Initiative. A monitoring and evaluation system has been established to report on these outcomes and decrease lost to follow up.
In the area of multi-drug resistant TB (MDR-TB), the Global TB Program has worked with the National Department of Health and local partners to update national guidelines for both drug sensitive and drug resistant TB. Finally, they have implemented these practice guidelines at the largest referral hospital in the country at Port Moresby General Hospital. Since 2014, the Baylor Global TB Program has worked side by side with staff to diagnose and treat 50 children with MDR-TB. Finally, the Global TB Program is working on ways to monitor and prevent children from acquiring MDR-TB.

In collaboration with partners from the University of the Philippines Manilla and Baylor’s National School of Tropical Medicine, the Global TB Program has implemented a community-based child TB initiative on the island of Bohol entitled ‘Diagnosis, Treatment, and Management of Pediatric Tuberculosis in Health Emergencies & Disasters’. Sponsored by the National Academies of Science USAID PEER Health program, our project employed rapid assessment methods to determine the prevalence of TB infection and disease in children. The project was further augmented by a descriptive study using social science mixed methods to assess barriers to pediatric TB control, prevention, and treatment post-disaster.

eSwatini
The fulcrum of the Global TB Program is based in Mbabane, eSwatini where we serve as a national referral center for pediatric TB and host a broad range of translational research projects. Our program has been developed to support cutting-edge diagnostic and immunologic research that will elucidate the pathophysiology of HIV-TB co-infection and inform the development of future preventive and treatment interventions.
The Global TB Program has made a substantial investment in the construction of a clinical, radiologic, and laboratory facility in Mbabane. The unique facility is situated on the grounds of the current Baylor College of Medicine Children’s Foundation – eSwatini Center of Excellence (COE) allowing for fully integrated HIV and TB care and treatment.

Tanzania
The Global TB program collaborates with our Tanzanian colleagues led by Dr. Jason Bacha, a faculty member at Baylor Tanzania-Mbeya, to improve pediatric TB diagnosis and care. Beginning with the development of a protocol for a medical records audit to review the COE’s experience providing integrated TB care to HIV-exposed, HIV-infected and HIV-uninfected infants and children and describe the clinical and operational outcomes of all children in whom Anti-Tuberculosis Treatment was indicated at the COE between Jan. 1, 2012 and Dec. 31, 2014. Collaborations continue to grow with projects using stool-based PCR to improve pediatric diagnosis of TB. Similarly, evaluation of differentially methylated host immune genes is evaluating improved TB diagnostics and future novel host-directed therapies.

Dr. Betty Nsangi, a clinical assistant professor at Baylor College of Medicine in Uganda and former AITRP fellow, received the Global Research Initiative Program for New Foreign Investigators award from the Fogarty International Center.
The R01 is titled, “Incidence, determinants and outcomes of latent and active TB among HIV-infected children.” The aim of the project is to determine the burden of latent and active TB and their treatment outcome among HIV-infected children in Uganda. This award assists her in developing her research platform and affords a platform for expanding new research collaborations.








