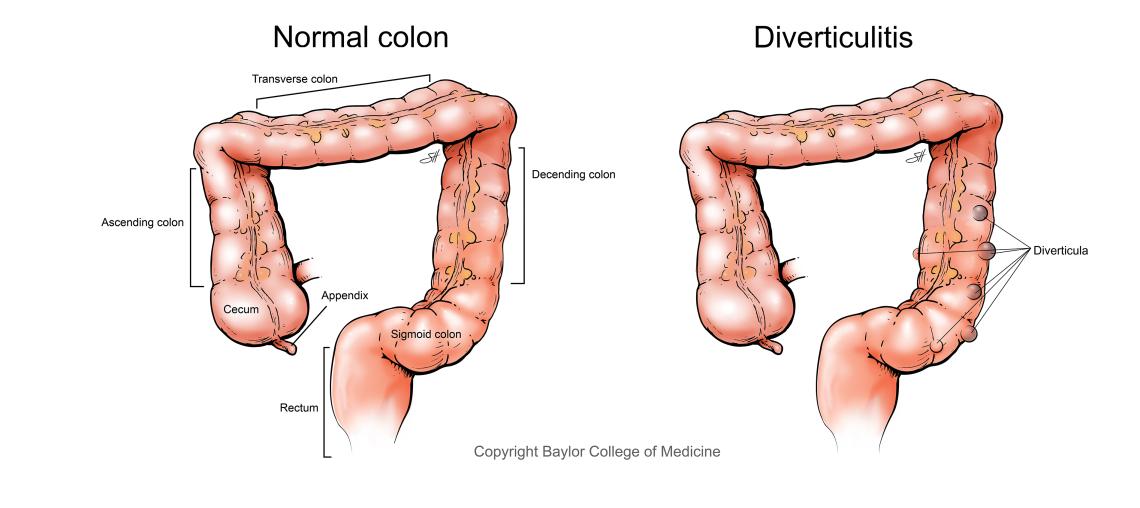
What is Diverticulosis and Diverticulitis?
Diverticula are small, bulging pouches that can form in the lining of your digestive system. They are most often found in the left lower part of the large intestine. The presence of diverticula is called diverticulosis.
When one or more of the pouches become inflamed, and in some cases infected, that condition is called diverticulitis. Diverticulitis can cause severe fever, abdominal pain, nausea and a noticeable change in your bowel habits.
Causes
- Diverticula usually develop when naturally weak places in your colon give way under pressure. This causes marble-sized pouches to protrude through the colon wall.
- Diverticulitis occurs when diverticula tear, resulting in inflammation and in some cases infection.
How is diverticulitis diagnosed?
When diverticulitis is suspected, your provider will look for it on imaging tests.
- A CT scan can show the extent of the inflammation as well as any related complications.
- I f you have not had a recent colonoscopy, this will be ordered six weeks from your last episode of diverticulitis.
Treatment for Diverticulitis
- Mild diverticulitis can be treated with changes in your diet and antibiotics.
- Recurring diverticulitis and/or complicated diverticulitis requires surgery, where the problematic section of the bowel is removed (colectomy). This might involve a temporary ostomy, which allows the body to recover safely from the diverticulitis and the surgery.
- With an ostomy, your intestine is moved to an opening in your abdominal wall, so your stool is collected in a bag. This bag collects the waste, and you can empty it when needed.
Your healthcare team will carefully evaluate your situation and recommend the most appropriate treatment. They’ll consider factors like your overall health, how often you have experienced diverticulitis and how severe those episodes were. If surgery is recommended, you will receive detailed instructions regarding your surgery and recovery.








 Credit
Credit