Dr. Zoorob presents at the European FASD Prevention Conference in London.
Overview of the Diagnostic Process
Interdisciplinary Evaluation
The management of fetal alcohol syndrome and fetal alcohol spectrum disorders starts with a diagnostic evaluation that consists of both making the diagnosis of an FASD and also ensuring that the family understands the individual's unique medical and neurobehavioral needs. A typical FASD evaluation is performed by a team consisting of a primary care clinician or developmental pediatrician, psychologist, social worker and speech-language pathologist. The team may also include an occupational therapist or educational specialist. There are pediatricians who can diagnose an FASD based on the Institute of Medicine recommendations (Institute of Medicine, 1996) or the CDC FAS Guidelines for Referral and Diagnosis (CDC, 2004). However, in many cases it is important to have a geneticist evaluate the individual for other genetic conditions that may be present in addition to an FASD or that could mimic the presentation of an FASD.
Because FASDs can affect the facial structure, growth, central nervous system, and other organ systems of the individual, appropriate medical referrals should be pursued as needed. For example, some individuals with FASD may have sensorineural hearing loss, vision problems or cardiac abnormalities that may require the help of additional specialists. Failure to thrive and short stature may require evaluation by a gastroenterologist, endocrinologist, and nutritionist. The FASD diagnostic process can be viewed as part of a continuum of care that helps identify and facilitate the appropriate health care, education and community services for the child and for the family. While there is no cure for FASDs, several strategies to mitigate secondary disabilities may be helpful for individuals and their families beginning in infancy and continuing through adulthood.
Assessment for Secondary Conditions
Individuals with an FASD are at risk for secondary conditions such as Attention Deficit Hyperactivity Disorder and anxiety that may necessitate psychopharmacologic intervention. In these cases, appropriate interventions include involvement from child psychiatrists, developmental pediatricians, neurologists and/or other mental health professionals. An interdisciplinary approach often helps in the overall management of a child with an FASD.
FAS requires documentation for ALL THREE of the following finding:
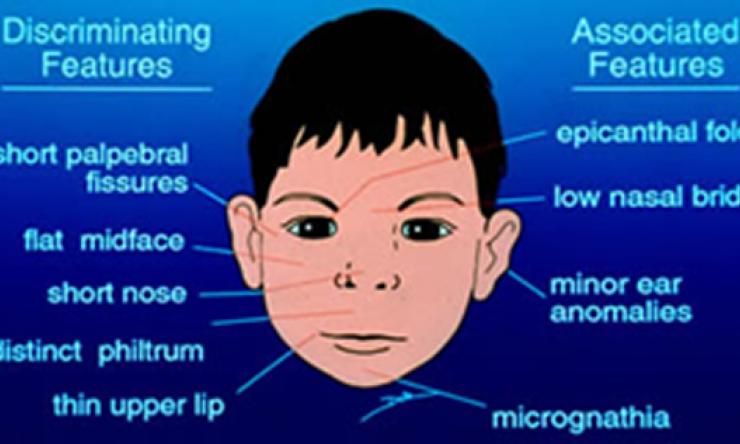
Three facial features or abnormalities including smooth philtrum, thin vermillion border, and small palpebral fissures. (Graphic below)
Growth deficits/problems
Central Nervous System abnormality
Note: Confirmed prenatal alcohol use can strengthen the evidence for an FAS diagnosis, but is not necessary in the presence of all other criteria.
Facial Features
Based on racial norms, the individual exhibits all three characteristic facial features:
Smooth philtrum (measured by Lip-Philtrum Guide Rank 4 or 5)
Thin vermillion border (measured by Lip-Philtrum Guide Rank 4 or 5)
Small palpebral fissures (at or below 10th percentile)
Neurological Problems
Neurological problems not due to a postnatal insult or fever, or other soft neurological signs outside normal limits.
Functional
Performance substantially below what is expected for an individual’s age, schooling, or circumstances, as evidenced by:
Global cognitive or intellectual deficits representing multiple domains of deficit (or significant developmental delay in younger children) with performance below the 3rd percentile (two standard deviations below the mean for standardized testing) OR Functional deficits below the 16th percentile (one standard deviation below the mean for standardized testing) in at least three of the following domains:
Cognitive or developmental deficits or discrepancies
Executive functioning deficits Motor functioning delays
Problems with attention or hyperactivity
Social skills
Other, such as sensory problems, pragmatic language problems, memory deficits, etc.
Growth Problems
Confirmed prenatal or postnatal height and/or weight at or below the 10th percentile for the child's age or sex, documented at any one point in time (adjusted for gestational age, as appropriate for race or ethnicity)








 Credit
Credit